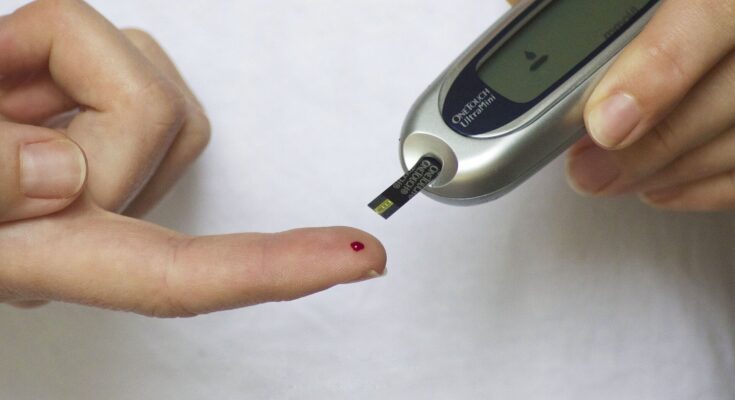
The most common reasons why people with type 2 diabetes (T2DM) are admitted to hospital with greater frequency than the general population are changing, with hospitalization for traditional diabetes complications now being accompanied by admissions for a diverse range of lesser-known complications including infections (i.e., pneumonia, sepsis), mental health disorders, and gastrointestinal conditions, according to an analysis of national data from Australia spanning seven years.
The findings, being presented at this year’s European Association for the Study of Diabetes (EASD) Annual Meeting in Stockholm, Sweden (19-23 Sept), reveal that just four traditional diabetes complications (cellulitis, heart failure, urinary tract infections, and skin abscesses) were ranked in the top ten leading causes of hospitalization in men and women with T2DM.
“Although traditional complications such as heart failure and cellulitis remain a substantial burden for people with T2DM, infections less commonly linked with diabetes and mental health disorders are emerging as leading causes of hospital admissions, and have substantial burdens that sometimes exceed the top-ranked well-known complications,” says lead author Dr. Dee Tomic from the Baker Heart and Diabetes Institute, Melbourne, Australia.
She adds, “The emergence of non-traditional diabetes complications reflects improvements in diabetes management and people with diabetes living longer, making them susceptible to a broader range of complications. Increasing hospitalizations for mental health disorders as well as infections like sepsis and pneumonia will place extra burden on healthcare systems and may need to be reflected in changes to diabetes management to better prevent and treat these conditions.”
While rates of traditional T2DM complications—including heart attack, stroke and amputations—have fallen substantially over the past 20 years in many high-income countries, driven by improvements in risk factors (e.g., blood pressure, cholesterol, smoking, and blood sugar control) and better preventive care and management, leading causes of death and illness such as cancer, liver disease and mental disorders are emerging among people with diabetes. In England, for example, classic complications accounted for more than half of hospitalizations in people with diabetes in 2003, but for less than a third in 2018.
Examining reasons for hospitalization at the population level can help identify emerging diabetes complications and increase our understanding of the burden of serious illness. However, little is known about the individual-diagnosis level reasons for hospitalization among people with diabetes across all diagnostic categories.
To find out more, researchers analyzed data from around 50% of Australians diagnosed with T2DM from the Australian Diabetes Registry (the National Diabetes Services Scheme; NDSS). In total, 456,265 individuals (aged 15 years and older) with type 2 diabetes registered on the NDSS between 2010 and 2017 were linked with hospital data and compared to over 19 million Australians aged 15 and above.
Modeling was used to identify the leading individual diagnosis-level causes of hospitalization among people with T2DM and to estimate the relative risk of hospitalization compared to the general population, after adjusting for age and calendar-year effects. Admissions for T2DM itself (eg, glucose disturbances such as hypoglycemia) were excluded from the analyses.
Diabetes complications were divided into three categories—traditional complications that included vascular diseases, kidney failure, retinopathy and cataracts, neuropathy, obesity, infections traditionally linked to diabetes (e.g., urinary), and complications of procedures related to well-known diabetes complications (e.g., amputation). Emerging complications included liver disease, mental health disorders, various cancers (e.g., gastrointestinal, female $ex organs), and infections less commonly associated with diabetes (e.g., respiratory infections, sepsis). All other diagnoses were categorized as ‘not commonly acknowledged’ complications.
Overall, the analyses found that people with T2DM are at greater risk of being hospitalized with most medical conditions compared to the general population (exceptions include prostate cancer, aortic aneurysm and wrist fractures).
The leading cause of excess hospitalizations in men with T2DM was cellulitis, responsible for 364 excess annual hospitalizations per 100,000 men with T2DM, followed by the lesser-recognized complications of stress disorders (241 per 100,000) and iron deficiency anemia (228 per 100,000)—with diabetes doubling the risk of admission for these conditions compared to the general population.
In women with T2DM, iron deficiency anemia was the leading cause of excess annual admissions (558 per 100,000), followed by the traditional complications of urinary tract infections (332 per 100,000) and cellulitis (267 per 100,000). High rates of excess hospitalization were also noted for lesser-known complications including depression (256 per 100,000), gastrointestinal disorders (237 per 100,000) and asthma (192 per 100,000)—with hospitalizations for asthma more than twice as likely amongst women with T2DM compared to the general population.
“The much greater risk for most mental health diagnoses in the diabetes population reinforces the evidence for mental health disorders as an emerging complication of T2DM,” says senior author Professor Dianna Magliano, Head of Diabetes and Population Health at Monash University, Melbourne, Australia. “The unexpected finding of a large burden of anemia in both men and women with T2DM suggests the possibility of a biological link between diabetes and iron deficiency. To look at this and other novel findings in more detail, we must conduct further analyses as diabetes registries become more common to understand the effects of diabetes on all organs to guide prevention and management strategies.”
The authors acknowledge that their findings show observational associations rather than cause and effect. They also note some limitations, including that the study included people from one high-income country with a predominantly white Caucasian population, so the findings cannot be generalized to low- and middle-income countries. Additionally, they were unable to exclude people with diabetes from the general population, so the strength of the associations might be reduced compared to an analysis of people with versus without diabetes.
EASD Stockholm 2022, Abstract 362: Cause-specific excess risk of hospitalisation in people with type 2 diabetes compared to the general population in Australia, 2010-2017
Edward W Gregg et al, The changing face of diabetes complications, The Lancet Diabetes & Endocrinology (2016). DOI: 10.1016/S2213-8587(16)30010-9
Jonathan Pearson-Stuttard et al, Trends in leading causes of hospitalisation of adults with diabetes in England from 2003 to 2018: an epidemiological analysis of linked primary care records, The Lancet Diabetes & Endocrinology (2021). DOI: 10.1016/S2213-8587(21)00288-6
Citation:
Reasons for hospital admissions in people with type 2 diabetes are changing (2022, September 1)
retrieved 2 September 2022
from https://medicalxpress.com/news/2022-09-hospital-admissions-people-diabetes.html
This document is subject to copyright. Apart from any fair dealing for the purpose of private study or research, no
part may be reproduced without the written permission. The content is provided for information purposes only.
Source link